“I can see the picture you got of yourself already... It’s a white house and you are Saint George complete in spotless armor. You get to a farmhouse. There’s this man bleeding to death. Now alone, without instruments, without assistance, you perform an impossible operation, and because your heart is pure, you save him. ”
I was in a hospital in London with kidney stones. My company, Circus Talents Ltd., had done successful tours for many of the biggest rock groups of the day. I was still unsatisfied. After all I never did become the drummer.
An old American film called “Not As A Stranger” came on the TV. The story followed a group of medical students’ as they became successful physicians. When Dr. Aarons, the supervising surgeon, spoke to the interns, I felt like he was talking to me. I had an epiphany. I would be like Dr. Runkleman, the small town physician with the big heart.
The desire to be a doctor had never gone away. It was just buried somewhere deep inside and the movie reawakened the dream.
I went back to the states and moved into my parent’s house. After all the years of Lear jets and limos, it was not easy living in the house I grew up in. I applied to colleges. After quite a few rejections, Hofstra University in Long Island, New York accepted me. I was a pre-med student all over again, but this time it was different.
I moved to a basement apartment close to school and I worked very hard. What should have taken three years or more, took two. Medical schools were not interested. I was too old and my story was too strange. To make matters worse there was a glut of applicants because of the GI’s coming back from Nam. I was not to be deterred. No one thought that I would succeed in the music business either.
Neil during his studies in Guadalajara, Mexico.
There were a few medical schools around the world accepting American students. I had a friend in the Philippines and another in Italy. I chose Guadalajara, Mexico. I knew some Spanish and the Guad(as we affectionately called it) had a good reputation.
It was very hard at first. Classes were one hundred percent in Spanish. Although I had taken a six-week language intensive, it wasn’t nearly enough. Eventually I found a group of bilingual Cubans. Even with their help, if my desire and determination had not been so strong, I never would have made it.
The best thing about going to school in Mexico was Mexico itself. We embraced the culture and unlike most U.S. students we didn’t isolate ourselves in an American neighborhood. It was our first taste of the third world and we liked it.
After medical school, in order to be eligible to take the licensing exams, I had to do a year of unpaid internship. It was a rude awakening. Medical training is like the army. I started as the lowest of the low (scut puppies as we were called, expected to do all menial medical tasks no one else wanted to do). The year went fast.
The operating room appealed to me and I was accepted into a 4 yr. surgical residency. Notoriously hard with every second or third night on call, it was a pyramid program. Each year a few more of us would be told not to return so that only two would remain at the end. No friends, no sleep, no fun!!!
As a second year surgical resident, I was able to moonlight in the emergency room of Queens General Hospital, a designated New York City trauma center. When someone came to the ER with a surgical problem I was the first one they saw. I treated victims of everything from auto accidents to building collapses. On the weekend it became the knife and gun club. Patients came through the door with wounds of every conceivable part of the body. I got really good at sewing and I liked the action. When I decided to leave surgery, ER medicine was a serious consideration. In the end, the hours and constant adrenaline rush convinced me to go another route.
The anesthesia residents were fascinated by my early rock and roll experiences. They particularly liked the drug stories. That was their area of expertise and I realized maybe mine as well. Many street drugs are versions of legitimate medications. For example heroin is the street version of morphine.
After two years of surgery, I switched to the other end of the operating table. Anesthesia residency was three years. I received one year of credit and I completed the training two years later. All in all it took me over 10 years from the time I left the music business until I was finally ready to hang a shingle.
I couldn’t see myself as a hospital based Anesthesiologist. There were a couple of anesthesia residents moonlighting in clinics and offices, but nobody doing it full time. They did it on the weekends and days off. I wondered if there was enough work to support myself.
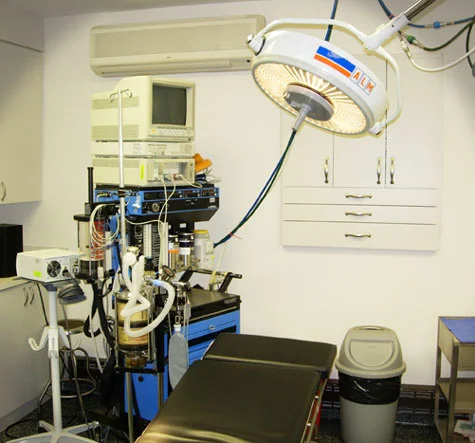
There were good reasons why most anesthesiologists had no interest in this type of practice. Out of hospital anesthesia was almost exclusively conscious sedation. Put in an IV, hook the patient to monitors, give periodic medications and observe. There were none of the bells and whistles of the complicated hospital based cases. On top of that, the drugs and the monitors were not good for that type of Anesthesia. Potentially, it was dangerous.
I was shunned by most of the legitimate anesthesia community.
“You can’t go in an office and give anesthesia without a team.”
“You better watch out, you are going to kill someone”
“You absolutely can’t do general anesthesia in an office.”
It became clear to me that cosmetic surgeons, if given the chance, would want to operate as much as possible in their office. The only thing holding them back was anesthesia. Most of them were giving anesthesia themselves in the office for small procedures, not an ideal situation. They dealt with famous clients who wanted as much privacy as possible. And the hospitals didn’t show them much love. Usually making them schedule at very inconvenient times.
I read about a well-known plastic surgeon in the gossip column of the New York Post. He worked in the hospital where I was finishing my residency. I approached him as he walked out of the OR.
“Hello Dr. Reed my name is Dr. Ratner."
“Hello Dr. Ratner, nice to meet you, what can I do for you?”
“Dr. Reed I have heard a lot about you. I know you are a very good plastic surgeon with a busy office practice. I would like to ask you a question.”
“Sure go ahead.”
“Who gives anesthesia in your office?”
“What do you mean? I give some sedation myself.“
“Yes I am sure you do, but don’t you have an Anesthesiologist come in for bigger cases?”
“No, I have to do the bigger cases in the hospital.”
“Dr. Reed wouldn’t you like to have an Anesthesiologist come to your office? I am sure the type of patients you deal with would prefer to have surgery in the privacy of your office OR.”
It didn’t take him long to reply.
“When can you start?”
As a musician I had the opportunity to observe people as they listen to music. The power of music is amazing. The right piece of music at the right moment can bring one single powerful emotion or a combination of many.
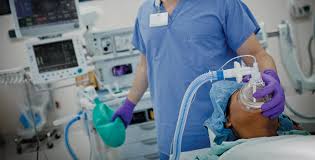
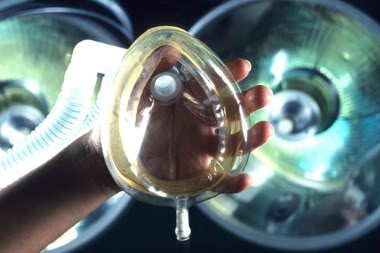
In the hospital, when the older anesthesiologists saw me put headphones on my patients they laughed at me. I knew better. Music was another drug in my cocktail. All my patients in the office got a set of headphones.
I was well trained and confident. I had a good background in business and I could relate one on one with most patients (a trait unfortunately absent in many of my fellow physicians).
The surgeons were amazed and most said that I was the best they had ever seen.
The monitors improved and the drugs got better. I didn’t kill anyone and my practice grew quickly. I proved the naysayers wrong. The specialty of Ambulatory Anesthesia grew out of these early efforts.
Anesthesia Dangers.
People die every year because of anesthesiologists’ errors. How not to be a victim.
Health confidential interview Neil Ratner, MD, director of anesthesiology at three New York ambulatory surgery facilities - the New York Surgical Center, the Reed Center for Plastic and Reconstructive Surgery and New York Fertility Institute. Health Confidential Magazine, September 1994.
When we need an operation, we spend time researching the best possible surgeon. But equally important to health and welfare is the skill of the anesthesiologist… and the type of anesthesia that will be used.
Because most surgeons work consistently with the same group of anesthesiologists and nurse anesthesists, you may not have much control over who administers the anesthesia. But you can ask your surgeon in advance for the name of the anesthesiologist whom he/she most frequently uses.
Next, contact your county medical society or state medical board to see if any lawsuits or complaints have been levelled against the anesthesiologist.
The existence of a few complaints or suits does not signal incompetence. But if the total number is 15 or more, further investigation is necessary.
Once you’re satisfied with the anesthesiologist, schedule a face-to-face meeting with him at least a day in advance of your scheduled surgery. Points to discuss…
- Find out what type of anesthesia will be administered. General anesthesia puts you to sleep, regional anesthesia numbs a large section of your body and local anesthesia numbs only the area surrounding the incision.
Caution: While local anesthesia may safely be administered by almost any doctor, nurse or dentist, any procedure involving general or regional anesthesia calls for the anesthesiologist to be on hand at all times to continuously monitor your condition. This applies even to minor diagnostic procedures. - Inform the anesthesiologist of all medical problems. That includes acute ailments (like cold or flu) and chronic problems (like food or drug allergies). You should also tell him if you take prescription or over-the-counter medications, or if you use alcohol, tobacco or illicit drugs.
Reason: These substances cause your body to react unpredictably to the various drugs used in anesthesia. Your anesthesiologist or anesthetist will use this knowledge to decide whether survey can be safely performed… or if it must be postponed. If your anesthesiologist is unaware of your habits or your overall health, you’re putting yourself at needless risk. - Determine what precautions should be taken. To reduce the risk of choking on vomit during anesthesia - a potentially fatal complication - avoid intake of all foods and liquids (including water and hard candies) for at least eight hours prior to surgery. To improve the condition of their lungs, smokers should cut out tobacco well in advance or surgery - at least 24 hours.
- Find out if music is provided for patients. Listening to soothing music in the operating room helps calm anxious patients before and during surgery. Music also speeds recovery. If the hospital does not provide music, make arrangements to bring your own tape player and headset.
- Use your mind to calm your body. Going into anesthesia is stressful. If you can calm your mind - through meditation and other methods - it will help your body relax and promote a more positive experience.
Illustration © D Yael Bernhard
Out From Under
Anesthesia is relatively safe. Still, when it comes to coming to, leave nothing to chance.
New York Daily News, Collete Bouchez, April 1994.
Each year, millions of surgical patients rely on anaesthesia to get them comfortably through an otherwise gruelling procedure. For most, the experience is safe.
But for some patients, things don’t work out well. Heart attack, stroke and even death can result from anesthesia-related complications.
Statewide in 1991, nearly 300 patients suffered complications from anesthesia - and 42 of them died, the state Health Department reports.
“We believe the actual number [statewide] may be a lot higher than what is being reported.” says department spokeswoman Vicky Zelbin.
The news that health officials are looking into several anesthesia-related incidents at St. Luke’s-Roosevelt Hospital in Manhattan has turned the spotlight on this highly eating medical science. The question on everyone’s mind:
How safe is anesthesia?
More than 25 million surgical procedures are performed annually in the United States. The number of anesthesia-related problems is thought to be less than 1 in every 100,000 cases, says Dr Elison Pierce Jr., professor of anesthesiology at Harvard Medical School.
The American Medical Association reports malpractice premiums for anesthesiologists have been about halved over the last decade - indicating problems with anesthesia are declining as well.
“With the advent of new monitoring devices and safer drugs, anesthesiology has emerged as one of the safest branches of medicine today.” says Dr. Neil Ratner, director of Anesthesiology at New York Surgical Center.
Still, doctors say if you are considering elective surgery, it is wise to take precautions.
First, meet with your anesthesiologist, well before your scheduled surgery.
“We encourage patients to meet with him/her as soon as their surgery date is scheduled, and to discuss a wide range of personal and family health issues related to anesthesiology” says Dr. Roberts A. Caplan, chairman of the Committee on Patient Safety and Risk Management for the American Society of Anesthesiologists.
What does your anesthesiologist need to know?
A personal and family health history, including any incidence of heart attack, blood pressure or hypertension, allergies to drugs, foods or environmental factors, history of chronic respiratory problems such as asthma, pneumonia or bronchitis, plus any cardiac symptoms you are experiencing, including rapid heartbeat or shortness of breath. Also, report any adverse reactions you or a family member has had to anesthesia in the past.
“This can help us to customise your anesthesia and avoid potential problems” says Caplan.
You should also relay information on any prescriptions drugs you take and on current or past use of “recreational” drugs, alcohol and cigarettes, says Ratner.
“These substances make a great difference in how a patient responds to and reacts under anesthesia” says Ratner.
Stopping smoking for even a day or two prior to surgery also helps insure a safer anesthesia experience, he says.
Both doctors say you can increase your safety odds by asking questions - about your anesthesiologist’s background and training, and about the hospital or out-patient clinic where your surgery will take place, especially regarding what safety equipment - like monitoring devices - will be provided.
“Don’t assume every hospital has the same facilities or that all outpatient clinics can offer what hospitals can; somethings they don’t” cautions Ratner.
Is one type of anesthesia safer than other?
The many drug combinations used for anesthetic purposes fall into one of three categories: general, which blocks all sensations of pain in the brain and renders you unconscious; regional, which blocks the pain response from a large group of nerves in an entire area of your body (like your lower half), and local, which blocks pain in a small specific area, like a tooth or a toe. “Unless the anesthesia is a mild local (like Novocaine), any risk factors which are present are pretty much equal no matter what type is used” says Ratner.
If you are unhappy with the anesthesiologist your hospital assigns, you might request a different doctor, talk to your surgeon about the possibility of using another facility or ask about bringing in your own anesthesiologist.
Finally, don’t assume that the person administering your anesthesia is an experienced, licensed practitioner. Some dentists and private physicians, Ratner believes, take unnecessary risks by allowing anesthesia to be administered by someone other than an anesthesiologist or a nurse anesthetist. While this is not illegal, Ratner thinks it is unsafe.
“Anybody can put you to sleep, but it takes very special medical skills to insure you wake up, so check those credentials” says Ratner.
To check the qualifications of a New York State anesthesiologist, call the Medical Licensing Bureau: 1-800-342-3729.
For more information on anesthesia options and safety precautions, write: American Society of Anesthesiologist, 520 N. Northwest Highway, Park Ridge, Ill. 60068.